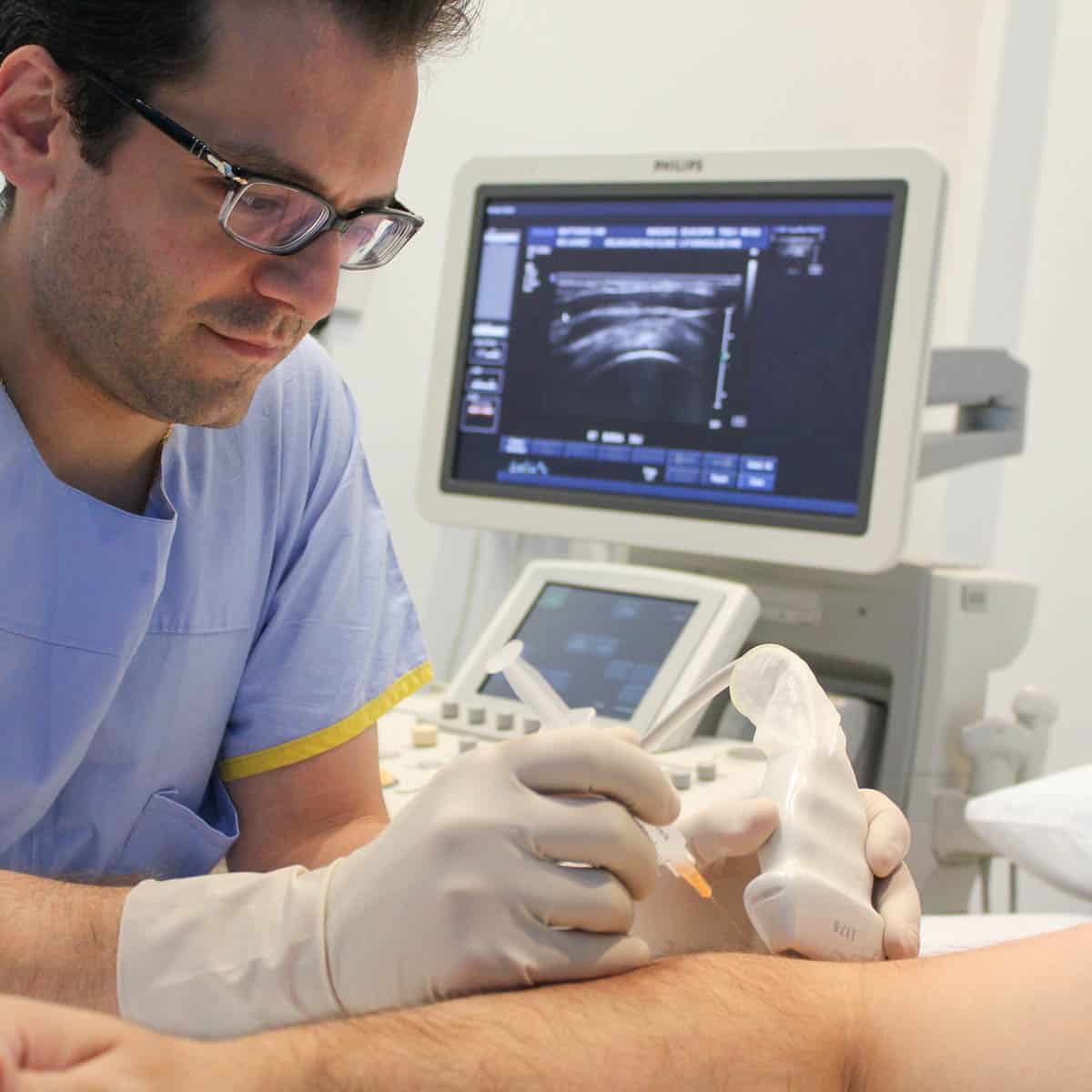
Pain Management Clinic Melbourne
Aches and pains are unfortunately a part of daily life, with most being self limiting and resolving spontaneously. When they persist and adversely affect our quality of life, then alleviating this pain becomes a priority for the patient and is a major clinical problem for doctors that requires an accurate diagnosis.
Given the morbidity of chronic pain, patients may benefit from the skills of a pain specialist.
With the help of a pain management clinic, Melbourne locals can be access treatment that will assist them on the path to recovery from injury, or at the very least, be able to manage any long term pain so that they can lead their lives with the best quality and function possible.

The Benefits of Attending a Pain Clinic
Melbourne pain management specialist can help patients with a huge variety of different conditions and diagnoses, with the aim of achieving excellent results when it comes to lessening pain and overcoming injury.
Types of pain management procedures performed at Melbourne Radiology Clinic include:
- Radiofrequency Ablation (RFA): This is where radiofrequency energy is used to produce an electrical current. This current results in heating areas of sensitive nerve tissue, disrupting the pain signals and therefore decreasing the sensation of pain. RFA can be used to treat joint pain and lumbar pain with excellent results. Pain relief can last for many months or even years.
- Spinal injections: A whole host of spinal injections are offered that can assist in the management of pain located to, and/or arising from the spine, such as:
- Facet joint injections
- Epidural
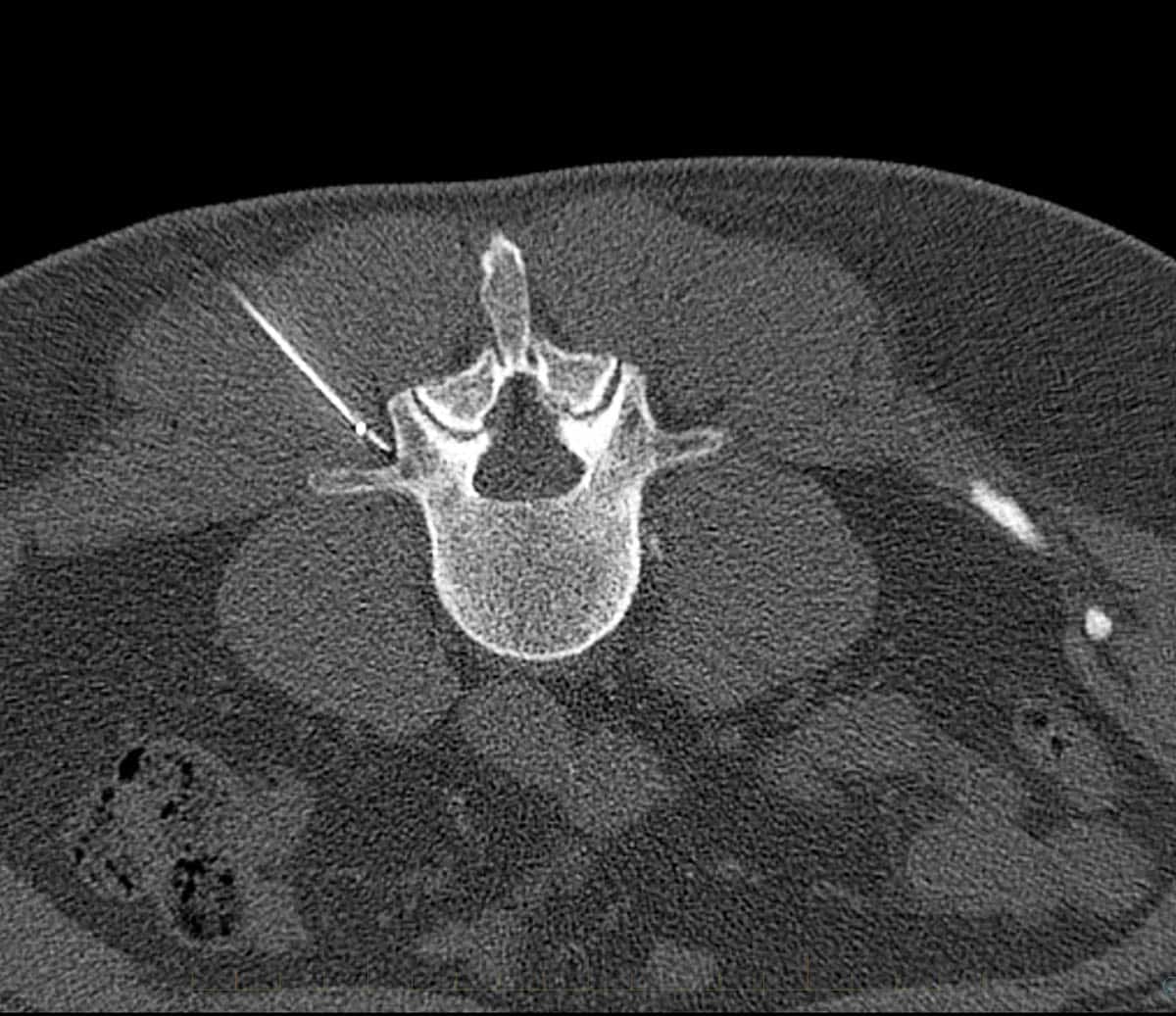
- CT guided nerve root injection
- Cortisone injection in foot
- Selective nerve root block
- Sacroiliac joint injections
- Sacrococcygeal joint injection and ganglion impar block
- General musculoskeletal injections: These assist in the treatment of conditions such as bursitis, arthritis, tendinitis/tendinosis and ganglion cysts, to name a few.
Pain management injections at Melbourne Radiology Clinic use modern imaging equipment for the accurate and safe delivery of pain relieving medication, using either ultrasound or CT guidance.
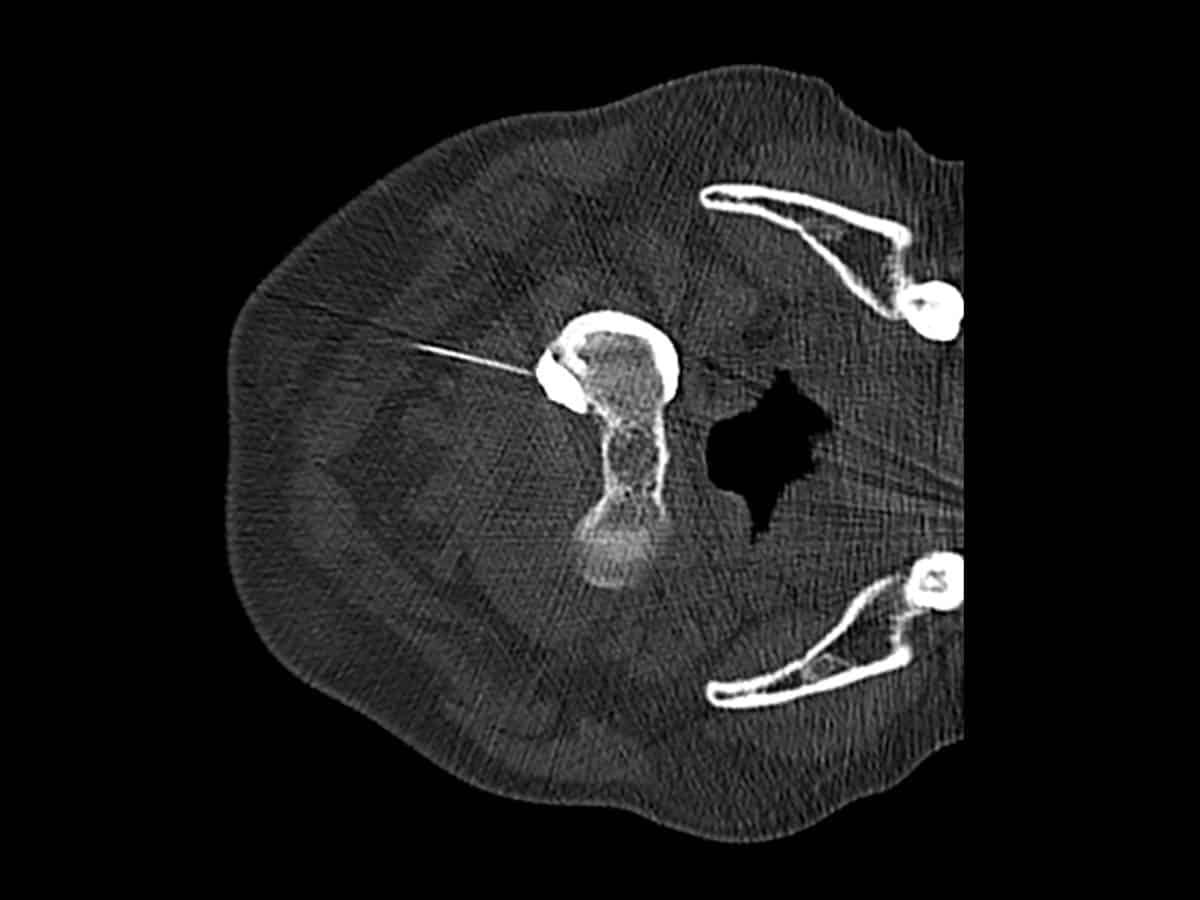
Pain Management at Melbourne Radiology Clinic
If you require any radiological examination such as MRI scans, bulk billing X-ray scans and/or procedure, then contact the team at Melbourne Radiology Clinic. We accept referrals from all over Melbourne – any written referral can be used, even if it is for another radiology provider. To book, call our reception staff on (03) 9667 1667. Alternatively, email to info@melbourneradiology.com.au, including your referral, if you have been provided with this, or you can use our online booking form to get in contact and we can call you back to book you an appointment.
Specialist Radiologists.