Shoulder Injuries.
Shoulder injuries are common in athletes of all ages.
Instability leading to dislocation (or near dislocation, known as subluxation) typically occurs in young people and is usually following a single traumatic episode, such as being tackled during a football game, or falling on an outstretched arm. Identifying which structures are injured and quantifying the degree of injury is important as the athlete may be a candidate for surgical repair and this is most accurately done with MRI. If the patient is unable to undergo an MRI, then a CT arthrogram may be used in its place.
Falling onto the point of the shoulder often results in disruption of a small joint above the shoulder known as the acromioclavicular joint, or commonly referred to as the AC joint.
Overuse, or ‘wear and tear’, injuries in combination with advancing age predisposes the mature athlete to tears of the tendons of the shoulder that stabilises the shoulder that are collectively known as the rotator cuff. The earliest spectrum of tendon injury is degeneration, or tendinosis (previously referred to as ‘tendinitis’), where daily damage sustained by the tendon exceeds the ability of the tendon’s internal capacity of repair. Further overuse may then lead to the development of partial and full thickness tears which may then progress to the development of partial thickness tears. Read More
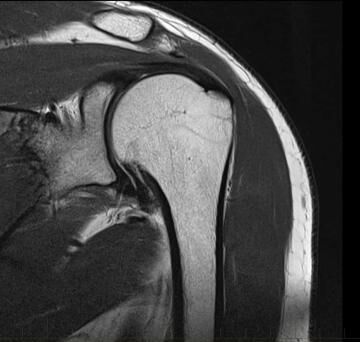
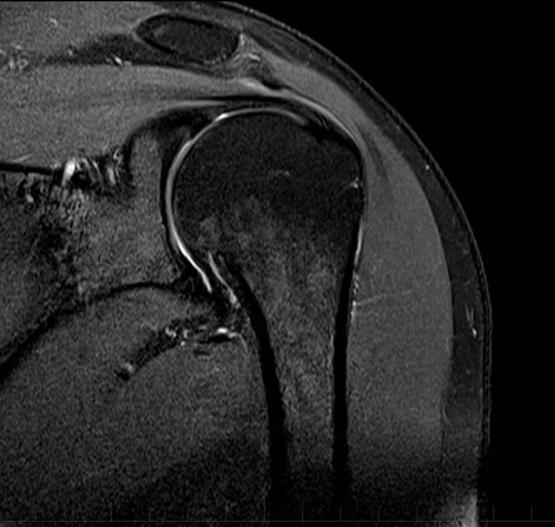
MRI & Xray for Shoulder Injuries
If you have suffered a shoulder injury, following an initial assessment by your doctor, you may require a radiological examination in order to determine the severity and the extent of injury.
Should I Get An Xray for Shoulder Injury?
An x-ray is ordered predominantly to exclude the presence of a fracture, as its is an accurate examination for the assessment of fractures as well as it being simple, quick and cheap. Other potential causes of your pain, as well as any associated soft tissue injury, as a general rule are not seen on an x-ray.
At Melbourne Radiology Clinic, we utilise the latest in digital imaging technology to perform x-ray for shoulder injuries, that results in simultaneous reduced radiation and superior imaging quality.
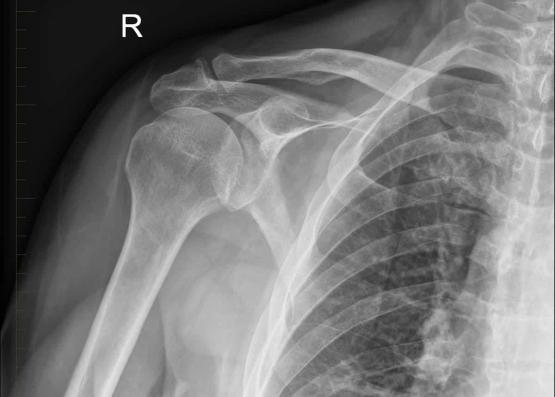
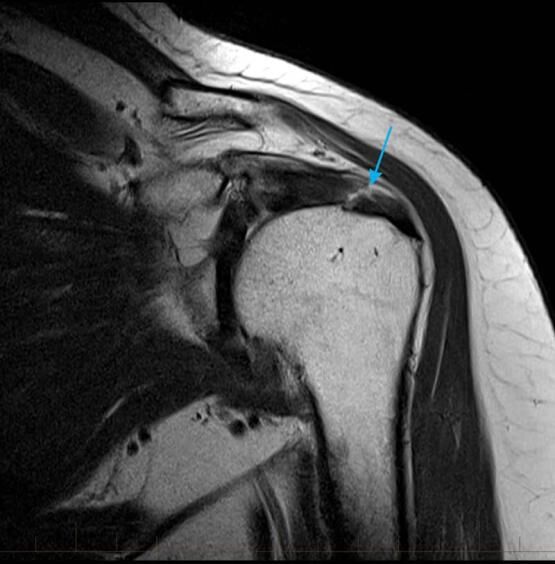
Should I Get An MRI of Shoulder Injury?
An MRI scan for shoulder injury will be able to identify and evaluate any soft tissue damage to the shoulder, such as traumatic injuries of the tendons, ligaments, muscles and cartilage, namely tears of the same. It is a non-evasive examination that typically takes 20 minutes to complete.
At the Melbourne Radiology Clinic, we utilise a Siemens Espree MRI unit that has a wide bore to ensure patient comfort throughout the scan.
No preparation is required for a shoulder injury MRI scan. When you arrive for your appointment, you will be asked to change into a disposable gown and remove any metallic devices. You will then be asked to lie down on the MRI scan table and lie throughout the scanning process in order to obtain the best image quality.
You can wear noise-cancelling headphones to distract yourself during the process, as well as music being played through these headphones. Our radiographer will keep you informed throughout the scanning process as to the progress of the scan as well as to keep in communication with yourself to ensure that you are comfortable.
After your scan, one of our expert radiologists will review the images and provide a formal written report with the diagnosis/diagnoses to your doctor. This report will be delivered within 24 hours or instantly, if requested by your referring health care provider.
Book Your MRI or Xray Scan For Shoulder Injury Today?
All appointments, except for x-rays, must be booked in advance at Melbourne Radiology Clinic. Book directly by calling us at the clinic or email to info@melbourneradiology.com.au, including your referral, if you have been provided with this.
Case examples:
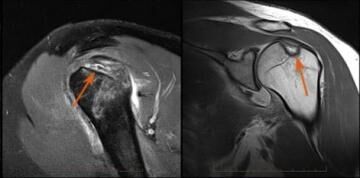
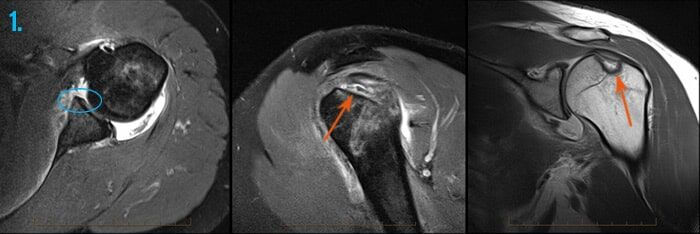
1. Shoulder dislocation
MRI evaluation following an episode of shoulder dislocation demonstrates focal absence of a specialised cartilaginous structure of the shoulder known as the labrum (circle) with a massive compression fracture of the humeral head (arrows) known as a Hill-Sach’s fracture.
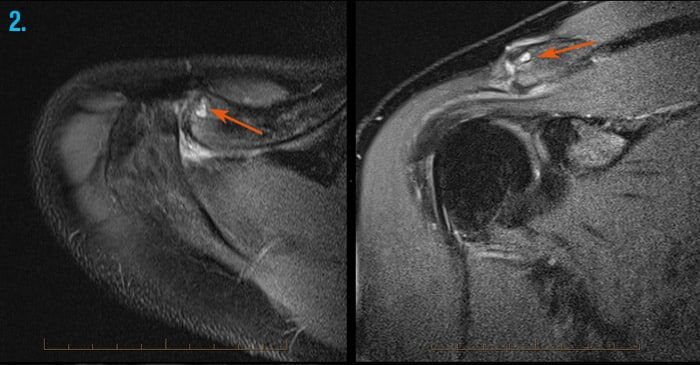
2. Acromioclavicular joint
MRI of the AC (acromioclavicular joint) demonstrates cyst formation and bone marrow oedema of the clavicle (arrows) consistent with clavicular osteolysis.
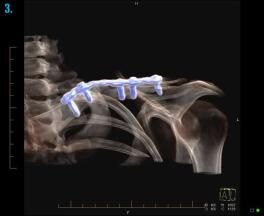
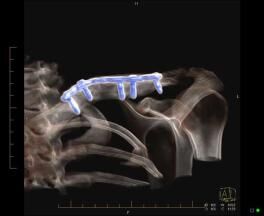
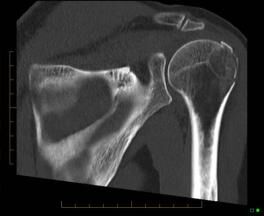
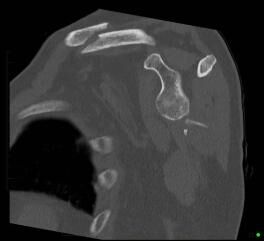
3. Use of CT Scanning in shoulder injuries
CT can be used to assess bone for fractures, focal lesions and in the post-operative patient where metallic hardware has been inserted
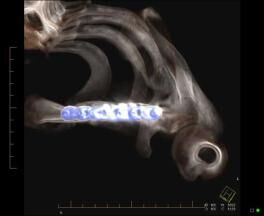
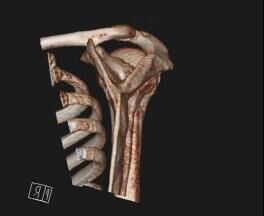
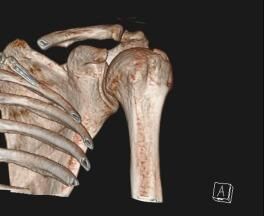
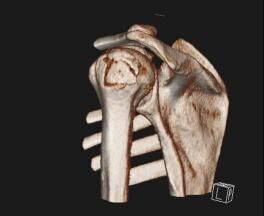
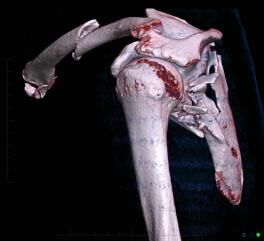
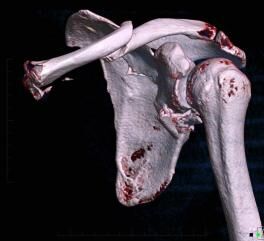
4. CT clavicle and scapula blade fracture
CT clavicle and scapula blade fracture with the source image showing the clavicle fracture and the 3D images showing the clavicle and the shoulder blade fracture